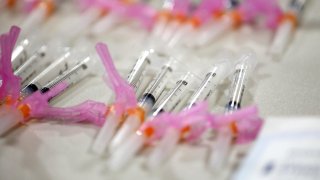
Public health officials sounded the alarm for months, complaining that they did not have enough support or money to get COVID-19 vaccines quickly into arms. Now the slower-than-expected start to the largest vaccination effort in U.S. history is proving them right.
As they work to ramp up the shots, state and local public health departments across the U.S. cite a variety of obstacles, most notably a lack of leadership from the federal government. Many officials worry that they are losing precious time at the height of the pandemic, and the delays could cost lives.
States lament a lack of clarity on how many doses they will receive and when. They say more resources should have been devoted to education campaigns to ease concerns among people leery of getting the shots. And although the federal government recently approved $8.7 billion for the vaccine effort, it will take time to reach places that could have used the money months ago to prepare to deliver shots more efficiently.
Such complaints have become a common refrain in a nation where public health officials have been left largely on their own to solve complex problems.
“The recurring theme is the lack of a national strategy and the attempt to pass the buck down the line, lower and lower, until the poor people at the receiving end have nobody else that they can send the buck to,” said Gianfranco Pezzino, who was the public health officer in Shawnee County, Kansas, until retiring last month.
Operation Warp Speed, the federal vaccine program, had promised to distribute enough doses to immunize 20 million people in the U.S. in December. It missed that target, and as of Friday, about 6.6 million people had received their first shot, according to a tracker from the Centers for Disease Control and Prevention. About 22 million doses have been delivered to states.
The American Hospital Association has estimated that 1.8 million people need to be vaccinated daily from Jan. 1 to May 31 to reach widespread immunity by the summer. The current pace is more than 1 million people per day below that.
U.S. & World
President-elect Joe Biden on Friday called the rollout a “travesty," noting the lack of a national plan to get doses into arms and reiterating his commitment to administer 100 million shots in his first 100 days. He has not shared details and was expected to discuss the effort this week. His office announced a plan to release most doses right away, rather than holding second doses in reserve, the more conservative approach taken by the Trump administration.
The Trump administration defined its primary role as developing coronavirus vaccines and delivering them to states, which would then take over and ensure that vaccine doses traveled “the last mile” into arms. Each state had to develop its own plan, including issuing guidelines for who gets vaccinated first. Several health experts complained about that approach, saying it led to confusion and a patchwork response.
“Let’s just say that I was disappointed how they handled testing, and the vaccine deployment has reminded me of how disappointed I was when they handled testing,” said Dr. Mysheika Roberts, health commissioner in Columbus, Ohio.
Several public health officials and experts say they believe some of the early glitches are smoothing out. Marcus Plescia, chief medical officer for the Association of State and Territorial Health Officials, said the slow start should not be surprising given the immense scale of the task.
“It was not going to be seamless,” he said.
Still, Plescia said the federal government could have done more ahead of the rollout — such as releasing billions of dollars earlier to help with staffing, technology and other operational needs.
An ongoing investigation by The Associated Press and Kaiser Health News detailed how state and local health departments have been underfunded for decades. Public health officials have warned since the spring that they lacked the staff, money and tools they needed to deploy a vaccine. The money was not approved until the end of December.
Vaccine distribution involves a long, complex chain of events. Every dose must be tracked. Providers need to know how much staffing they will need. Eligible people must be notified to schedule their shots, given the vaccine's handling requirements and the need to observe people for 15 minutes after the shot — all while social distancing is observed.
It’s difficult to plan too far ahead because the number of doses the state receives can fluctuate. Hospitals cannot give all their workers shots on the same day because of possible side effects and staffing issues, so they must be spaced out.
Rhode Island health officials said it can take up to seven days to get doses out to people once they are received. Officials in several states, including Rhode Island, Pennsylvania, Kentucky and New Jersey, said the lack of supply is one of the biggest obstacles to getting more people vaccinated.
Some communities have seen large numbers of medical workers put off getting the shot, even though they are first in line. Columbus, Ohio, has had lower-than-expected demand among top priority groups, including emergency medical workers.
A public education campaign could have helped address the hesitancy among health care workers that has slowed the rollout of the first shots, said James Garrow, a spokesman for the Philadelphia health department. Instead, officials for months talked about the speed at which they were developing the vaccines — which did not help alleviate concerns that it might not be safe.
“There just hasn’t been good messaging about the safety and the purposefulness of the safety protocols,” Garrow said.
The federal government has done little to provide information resources that local officials can tailor to their own communities, to address concerns of people such as pregnant women or Black men living in rural areas, said Dr. Michael Osterholm, an infectious disease expert at the University of Minnesota, who is a member of Biden’s COVID-19 advisory board.
“You don’t need 50 different states trying to do this kind of work. What you want to have is a smorgasbord of information sources that address different populations that any one state can use," Osterholm said. "That's what we don’t have right now.”
Some states are getting creative. Oregon held a mass vaccination event at the state fairgrounds with the help of the National Guard. The governor said it aimed to vaccinate 250 people per hour. New Jersey planned to open six vaccine “megasites” where officials hope more than 2,000 people per day can eventually get their shots.
But without a federal plan, such efforts can amount to “throwing spaghetti at a wall to see what sticks,” said Chrissie Juliano of the Big Cities Health Coalition, which represents metropolitan health departments.
What's needed is a national, wartime-type effort to get vaccines out to as many people as possible, multiple experts said. Medical emergencies can be covered 24 hours a day, seven days a week, said Pezzino, who is also a senior fellow at the Kansas Health Institute. Why not make vaccinations available on that schedule?
“It is possible. It is feasible,” he said. “I don’t see the level of urgency, the feeling of urgency in anybody around here. And that’s really, honestly, that’s the only thing that could make a difference."
Associated Press Writer Ricardo Alonso-Zaldivar also contributed to this report.



