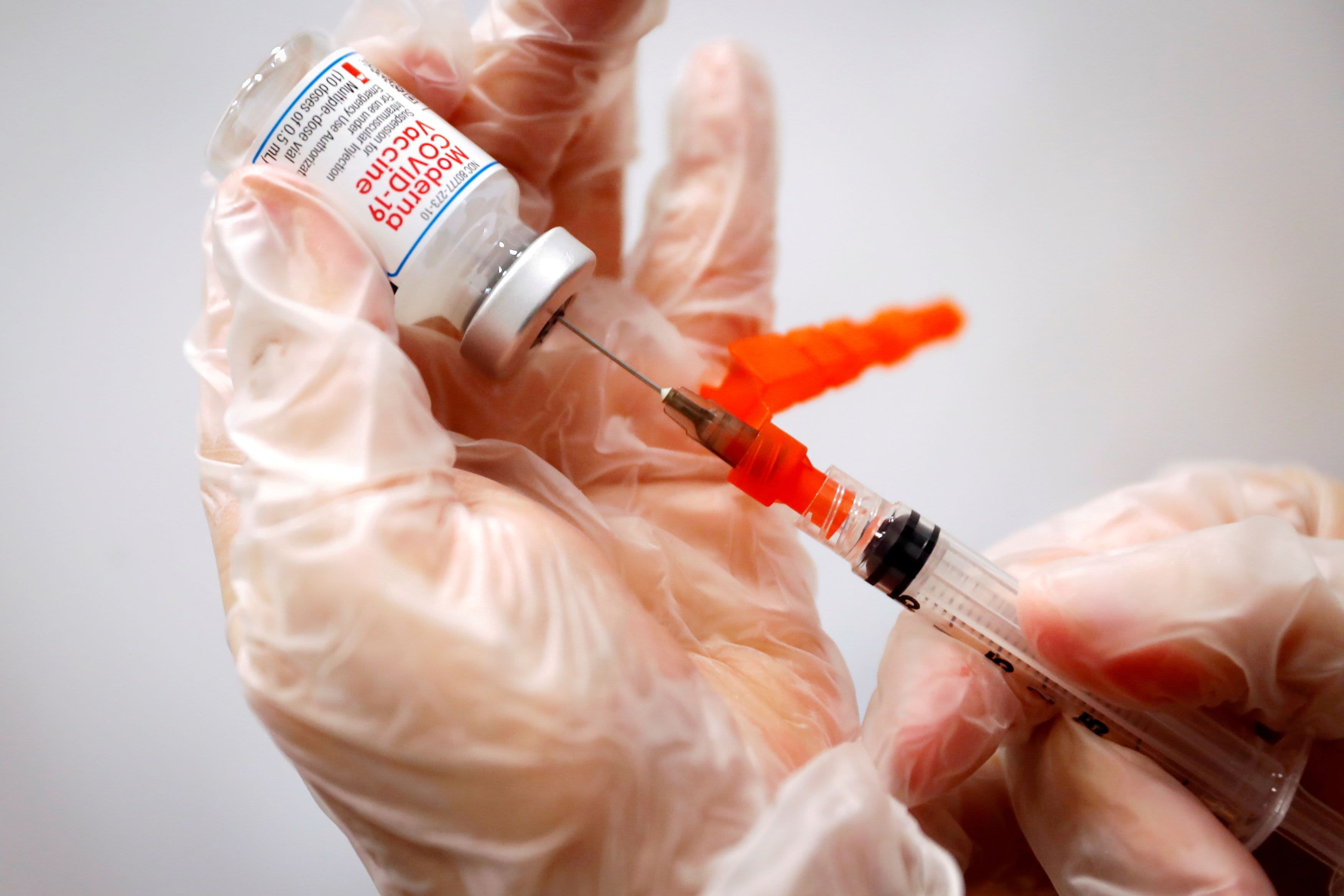
COVID-19 hospitalizations in Florida have increased by more than 365% in the last two weeks, and more than 90% in one week, according to the latest data from the state.
Hospitalizations rose from about 5,000 COVID patients to about 8,500 over the past week, according to federal government data. Cases in the state have continued to rise, reaching another record of 76,887 daily cases on Friday, CDC data shows.
At Jackson Health, officials said there's been a 258% in patients with COVID-19 in the last two weeks, with 500 patients as of Friday afternoon.
The Hurricane season is on. Our meteorologists are ready. Sign up for the NBC 6 Weather newsletter to get the latest forecast in your inbox.
At Baptist Health, there are currently more than 765 patients — a 370% increase in two weeks.
Meanwhile, Florida’s seven-day average in deaths is at its lowest level since March 2020, with four deaths per day.
COVID-19 LATEST
More than 40 Florida hospitals are facing staffing shortages as infections and hospitalizations continue to rise fueled by the omicron variant of the coronavirus.
Hospital groups say there are growing concerns as more medical staff gets infected with the virus even after being vaccinated, and doctors and nurses need to be isolated and off duty.
The omicron variant spreads even more easily than other coronavirus strains. It also more easily infects those who have been vaccinated or had previously been infected by prior versions of the virus. However, early studies show omicron is less likely to cause severe illness than the previous delta variant, and vaccination and a booster still offer strong protection from serious illness, hospitalization and death.
Though coronavirus infections have surged in Florida as omicron becomes the dominant strain, deaths in the state have continued to decline — to their lowest levels since the pandemic was just getting started in early 2020.
Justin Senior, CEO of the Florida Safety Net Hospital Alliance, which represents some of the largest hospitals in the state, said that this variant was infecting more staff members, requiring them to be isolated and off work.
Senior also said that although as many as 50% patients in some networks were arriving at the hospital for other ailments or procedures and then testing positive for COVID-19, those cases were still difficult to manage.
“They are really labor-intensive. To prevent further infections, they tend to be an immense amount of work that is very tedious,” Senior said.
The chief medical officer of Cleveland Clinic in Weston, who said their number of cases doubled in the last seven days, also named this a notable difference amid this surge.
"We’re not seeing the ICU cases, our admissions for COVID are typically to a regular nursing floor. We just have not seen the ICU cases, which is very beneficial to us, but we have seen an increase to our regular nursing floor," Dr. Scott Ross said. "I think it's a valid point that we’re seeing COVID being diagnosed on patients admitted for other non-COVID reasons. But at the end of the day, to take care of a COVID patient regardless of whether they're admitted for COVID or not COVID, it is more labor-intensive."
Get updates on COVID-19 in your inbox. Click here to sign up for our weekly coronavirus newsletter.